 
Increased plasma hs-CRP was associated with an increased number of metabolic syndrome components as defined by ATP III guidelines (i.e., central obesity, elevated plasma triglycerides, low plasma HDL-C, hypertension, & elevated blood glucose). 8 Plasma hs-CRP measurement was also found to aid risk prediction in 14,719 WHS participants with metabolic syndrome. Similarly, in the Women’s Health Study (WHS N ≈ 28,000), baseline plasma hs-CRP was superior to baseline plasma LDL-C for predicting first cardiovascular events over a mean of eight years. In the Physicians’ Health Study, elevated plasma CRP was associated with increased relative risk of MI in apparently healthy men, regardless of total cholesterol-to-high-density lipoprotein cholesterol (HDL-C) ratio. However, it may also be produced by vascular sources, including cells residing in atherosclerotic plaques.ĭata from several prospective studies demonstrate that baseline plasma CRP levels predict the risk of future cardiovascular events in apparently healthy people, adding prognostic value beyond that of plasma lipids. It also exhibits activities that may directly affect vascular disease, such as activation of the complement system. 6,7ĬRP provides a functionally integrated assessment (exactly for what we are looking in Functional Medicine) of overall upstream cytokine activation. 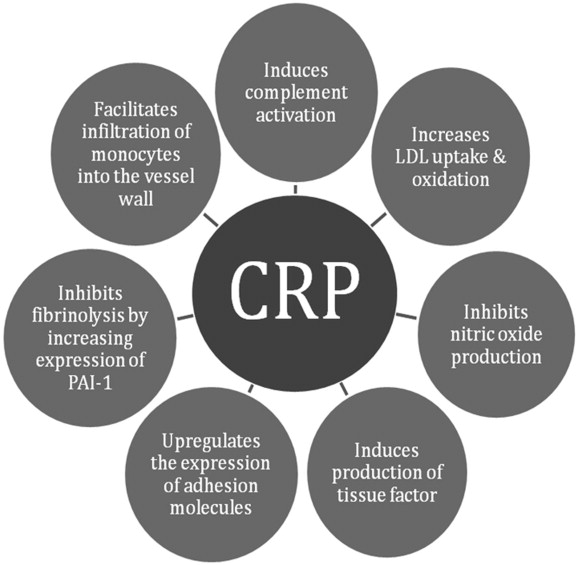
4,5 Plasma CRP has a long half-life in the circulation (~20 hours), high stability, and negligible circadian variability, and can be measured inexpensively using standardized high-sensitivity assays. The large increases in circulating levels of plasma CRP and serum amyloid A indicate major changes in the regulation of these genes as they respond to inflammation.Īlthough circulating levels of several inflammatory mediators correlate with increased coronary risk, CRP has attracted particular attention. These cytokines also stimulate production of interleukin 6 (IL-6), which stimulates the liver to produce acute-phase proteins, including CRP and serum amyloid A. 3 Systemic or local inflammation in blood vessels or tissue likely results in production of multipotent, primarily proinflammatory cytokines capable of inducing endothelial and other cells to produce adhesion molecules, procoagulant factors, and other mediators released into the circulation in soluble form. There is a pathway of inflammation that results in higher concentrations of various markers in peripheral blood. Therefore, Inflammation is essential to the formation of both atherosclerosis and its thrombotic complications. The inflammatory response also inhibits collagen production whilst stimulating macrophages to express tissue factor, a potent procoagulant. In turn, foam cells secrete additional inflammatory mediators that amplify inflammation in the vessel wall and weaken the protective fibrous cap of atherosclerotic plaque. The macrophages end up becoming foam cells after expressing scavenger receptors that allow them to engulf and modify lipoproteins. Endothelial cell expression of macrophage colony stimulating factor (M-CSF) further contributes to atherogenesis by promoting the conversion of monocytes into macrophages in the areas of this inflammation. This causes immune cells and smooth muscle cells to migrate to inflamed areas and increase in number. This inflammatory response results in endothelial cell activation, a condition in which endothelial cells begin secreting increased amounts of proinflammatory chemicals such as vascular cell adhesion molecule 1 (VCAM-1) and monocyte chemoattractant protein 1 (MCP-1). Arterial damage triggered by factors such as accumulated low-density lipoprotein ( LDL), oxidative stress, hyperhomocysteinemia, and hypertension can lead to an inflammatory response. Patients with higher hs-CRP concentrations are more likely to develop stroke, myocardial infarction (MI), and severe peripheral vascular disease.Ītherosclerosis is essentially a disease of chronic inflammation in the blood vessel. Elevated levels may be caused by any medical condition resulting in inflammation, infection, or primary/secondary tissue injury. High sensitivity C-reactive protein (hs-CRP) is an acute-phase protein that increases in response to various inflammatory stimuli (e.g., trauma, infection, arthritis, and surgery).ĬRP is a nonspecific inflammatory marker. Elevated levels of CRP are very common and most patients in our Tulsa, Oklahoma Functional Medicine Clinic want to know what they can do to reduce it. C-Reactive Protein (CRP) is a blood test in our basic metabolic lab panel. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
